
The reported incidence of CSF leak requiring intervention after spinal tumor surgery varies widely (0–28.6%) ( 3- 5, 47- 67), but a review of the recent literature would suggest that the overall incidence after surgery for both intradural and extradural pathologies is relatively low ( 68- 77) (mean, 6.6%±5.8% Tables 1,2 ). 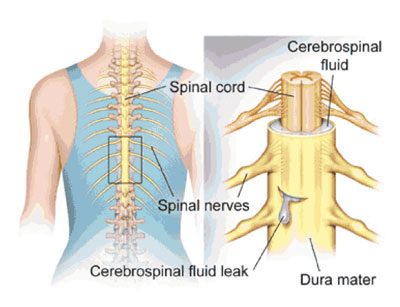
The goal of this article will be to review the literature on post-operative CSF leaks after surgical intervention for spinal tumors-with an emphasis on avoidance, recognition and effective management. Early identification and treatment of CSF leaks is necessary to avoid compounding the risks of spine tumor surgery and achieving the best possible patient outcomes. Inappropriately managed CSF leaks subject spine tumor patients to a number of associated complications, lengthened hospital stays, the need for additional interventions, increased health care costs ( 43, 44), and the propensity for tumor seeding ( 4, 45, 46). Patients undergoing surgical intervention for spinal tumors would seem particularly prone to the development of post-operative CSF leaks due to a number of factors, including: (I) the variable presence of an intradural tumor component requiring durotomy as a part of the intervention, (II) deficits in wound healing capability as a result of malnutrition, complex wounds, medical comorbidities, extended use of high-dose steroids or the need for adjuvant chemoradiotherapy, and (III) the use of anterior/ventral approaches to the spine which may create communications between the subarachnoid space and negative pressure potential spaces (e.g., the pleural cavity). The adverse outcomes of perhaps greater interest are post-operative CSF leaks that require secondary intervention and lead to CSF-leak-related sequelae after spine surgery, as these are a source of considerable patient morbidity and economic burden ( 43, 44). While unintended durotomies may lead to longer operative times, a delay in mobilization after surgery, and occasional nerve root injury or neurological deficit ( 30, 31), the majority of incidental durotomies are identified and addressed intraoperatively without the need for reoperation or further intervention, and evidence regarding the overall effect of incidental durotomy on long term patient outcomes are conflicting ( 19, 22, 40- 42). Unintended durotomies are reported to occur in up to 16% of spine surgeries in several large series ( 14, 15, 18- 38), with smaller series reporting even higher incidences ( 39). Accepted for publication Jan 02, 2019.Ĭerebrospinal fluid (CSF) leaks are a known complication of spine surgery, and an effective protocol for prevention, recognition and treatment of postoperative CSF leakage is essential to avoiding a cascade of associated adverse outcomes, such as durocutaneous fistula, wound infection ( 1- 5), intracranial hemorrhage ( 6- 12), arachnoiditis ( 13, 14), nerve root incarceration/strangulation ( 15, 16) and meningitis ( 3- 5, 17). Keywords: Durotomy cerebrospinal fluid leak spine tumor duraplasty dural repair In this article, the incidence, risk factors and complications of CSF leaks after spine tumor surgery are reviewed, with an emphasis on avoidance of post-operative CSF leaks, early post-operative identification and effective secondary intervention. Intraoperative identification of unintended durotomies and effective primary repair of dural defects is an important first step in the prevention of post-operative CSF leaks, but in patients who develop post-operative pseudomeningoceles, durocutaneous fistulae or other CSF-leak-related sequelae, early recognition and secondary intervention are paramount to preventing further CSF-leak-related complications and achieving the best patient outcomes possible. Post-operative CSF leaks increase morbidity, lengthen hospital stays, prolong immobilization and subject patients to a number of associated complications. Policy of Dealing with Allegations of Research MisconductĪbstract: Post-operative CSF leaks are a known complication of spine surgery in general, and patients undergoing surgical intervention for spinal tumors may be particularly predisposed due to the presence of intradural tumor and a number of other factors. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
